
Resources for Patients Starting or Continuing NINLARO® (ixazomib)
A variety of resources are available for both healthcare providers and patients.
Resources for your patients
NINLARO Treatment Calendar
Patient Experience Guide

Packaging
Instructions

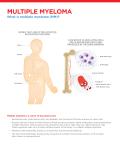
SLiM CRAB Tear Sheets for Patient Lab Test Education
Takeda Oncology Here2Assist® Brochure

NINLARO Patient Support Community

Resources for healthcare professionals
NINLARO Regimen Dosing Guide for Healthcare Professionals

Takeda Oncology Here2Assist® Enrollment Form

Lab Test Booklet for Healthcare Professionals

Convenient NINLARO Packaging

Instructions for patients taking NINLARO on the go
Share this helpful video with your patients so they can better understand how to take NINLARO at home or on the go.
Looking for more patient resources?
Find additional resources and support that could benefit your patients.
